It is a well-known fact that the population in Asia is aging. In this region, the proportion of the population aged over 65 is predicted to nearly double, from 7.73 percent in 2015 to 15.49 percent in 2035. Asia accounted for only 44 percent of the global older adult population in 1950, but by 2050, this share is projected to increase to 62 percent. Simply put, within the next few decades, Asia is poised to become the oldest region in the world.
Older age brings with new opportunities – opportunities to pursue new activities in the form of further education and exciting career extensions and also contribute in many ways for family members and give back to society through acts of volunteering. Yet the extent of these opportunities and contributions crucially depends on one factor: good health. As populations age, chronic health complications such as cancer, diabetes, and heart disease rise in tandem – and older adults may be at an increased risk of developing health complications as a consequence of infectious disease too.
The United Nations has proclaimed 2021-2030 to be the Decade of Healthy Aging, to improve the lives of older people, their families and communities – including changing perceptions toward age and aging and delivering people-centric integrated primary health services geared to older adults. An equally important and complementary strategy is that of the World Health Organization’s Immunization Agenda 2030. Under this strategy, the focus is on ensuring that everyone, everywhere, at every age, fully benefits from vaccines to improve health and wellbeing – including older adults.
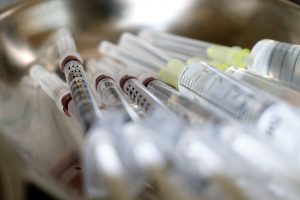
Immunization is one of the greatest success stories of modern medicine, preventing approximately 2 to 3 million infectious disease deaths every year across age groups and infection types, ranging from diphtheria, tetanus, whooping cough, influenza, and measles. In recent times, COVID-19 has shown us just how important immunization is; world-wide human and economic health quite simply depend on it. Immunization against all vaccine-preventable illnesses, including influenza, is just as essential to healthy aging.
However, life-course immunization, or routine vaccination throughout different life stages beyond pediatric vaccinations, is a significantly under-utilized public health intervention in many countries across the Asia-Pacific. Unlike in the United States and Europe, in many Asia-Pacific countries the importance of routine vaccination options beyond childhood are not well-recognized by policymakers nor well-understood by adult populations, and subsequently adult elective vaccination rates are very low, worryingly so for older adults and the more vulnerable.
This World Immunization Week must be the beginning of desperately needed action toward 2030 goals. It’s a time to reflect on the problem – but the more immediate need is faster and more sustained action.
The Scale of the Problem
Despite the benefits of vaccination being widely recognized as one of the most effective and cost-saving public health interventions, life-course immunization uptake rates remain low across the Asia-Pacific. In Singapore, for example, less than 15 percent of those aged 65 and above have taken the influenza vaccine, and across Asia, the median uptake is also less than 15 percent among the general population – far below the World Health Organization target of 75 percent.
The recent expert multi-disciplinary sustainable healthcare delivery and financing workshops conducted by Sanofi and KPMG in the Asia-Pacific region, with the support of World Economic Forum, showed that the biggest barrier to vaccination uptake is that most adults are simply not aware of its importance, and the misconception that crucial vaccines are only given at birth or to children. Additionally, the general population do not fully understand – and are faced with uncertainties about – the efficacy of vaccination or its components.
The Action We Must Pursue
The following three pillars are critical for the region to collectively address the challenges hindering life-course immunization, and to put life-course immunization on the healthy aging agenda.
First, the value of vaccinations in adult populations needs to be recognized, starting with immunization being integrated into national level healthy living and healthy aging policies. National immunization schedules should be updated to cover the whole life course, and recommendations should be evidence-based and regularly reviewed. In line with these schedules. National guidelines also need to be updated, especially when it comes to the vaccination of vulnerable populations.
The United Kingdom has made flu vaccines available for free to those aged 50 and above. In 2020, three-quarters of people in this age group received the free vaccine. The U.K. government places high importance on flu vaccination in adults, and the corresponding uptake among the target age group shows how public recognition of the value of the vaccine translates into higher vaccination rates.
Having a robust database to collect and share immunization rates and corresponding outcomes, such as drops in hospitalizations and morbidity, can further ensure that public health and healthcare professionals better recognize the tangible and positive outcomes of life-course immunization.
Second, and related, we must clearly communicate the value of life-course vaccinations. While the role of childhood vaccinations is clear, and many countries have compulsory vaccination schedules and mechanisms for delivering vaccines effectively to a pediatric population, the challenge is more elusive for adults and older adults. Beyond needing a motivation to seek vaccination that is not government mandated, understanding what the vaccine is for and how the vaccination works is crucial to increasing vaccine confidence, and subsequently uptake among the adult population. There is a need to provide neutral and factual information around the role, effectiveness, and risks of vaccination, along with information on access in order to empower individuals to make informed choices at different life stages, for themselves and for loved ones.
Outside of Asia, the United States and the United Kingdom are good examples of clear and transparent communication around the role, effectiveness, and risks of vaccination. Specific to the flu vaccine, both countries actively provide public information and resource packs on the types of vaccinations available and who should get vaccinated, among other information.
However, neutral and factual information can be overshadowed by the spread of misinformation, falsehoods, and conspiracy theories, which are creating fear, confusion, and reduced trust in the importance of vaccination. We also now have the more recent issue of social media spreading misinformation at an alarming rate, to the point of the World Health Organization has coining the term “infodemic.”
That said, social media and social influencers can still be effective touch points where the public search for information related to vaccinations. For example, in Hong Kong, social media analytics have been used to identify population subsegments against vaccination who are then targeted for education campaigns.
Communication is also key when it comes to the authenticity and integrity of vaccines, where timely, transparent, and accurate information is needed to counter any misinformation or challenges that arise.
Finally, we must implement novel models of sustainable healthcare funding. With growing public financing pressure and an increasing demand for healthcare services, there is an urgent need to identify innovative, pragmatic, and scalable ways to address crucial public health financial capacities, including for life-course immunization.
The traditional approach of relying on income taxes for public health spending has proven to be inadequate and unsustainable. Few countries in the Asia-Pacific region achieve the 15 percent tax-to-GDP ratio, the critical threshold set by the IMF to support sustained and inclusive growth. In addition, Asia’s aging population and shrinking workforce means that this taxable pool will further decrease. There are several non-traditional ways in which healthcare can be sustainably funded such as debt financing through public and private partnership in the form of Social Impact Bonds (SIBs), crowdfunding, and moving to a “pay-for-performance” model. One of the mechanisms could be to consider earmarking taxes or establishing nationalized funds for high-impact disease and treatment areas like immunization and RSV, the most common cause of hospitalization for Lower Respiratory Tract Infection (LRTI) in children younger than five years of age. For example, Taiwan earmarked sin taxes to procure new vaccines for its national immunization programs, while Bhutan invested its National Immunization Fund so as to reap the returns from the interest rates.
While there are many ideas and approaches to increasing uptake of life-course immunization, the most significant determinant of success criteria is the actualization of these ideas. Collaboration among diverse stakeholders across the healthcare ecosystem is integral to ensuring that the successful uptake of life-course immunization comes to fruition.
As the World Health Organization says, for over 200 years, vaccines have protected us against diseases that threaten lives and prohibit our development. With the help of vaccines, we can progress without the burden of diseases, which cost humanity hundreds of millions of lives. This World Immunization Week is a reminder that vaccines work – not just against COVID-19 but also in protecting people of all ages against various other diseases. We must look beyond the pandemic to increase trust and confidence in vaccines, in addition to investments in vaccines to remove the barriers to access in order to build solidarity and trust in vaccination as a public good that saves lives and protects health.